Do I Need Surgery for My Lower Back Pain or Herniated Disc?
To start, the answer to this question should be answered solely by a proper medical professional. If you are actively seeking treatment for lower back pain or disc herniation, make sure that your physician is actively involved in the treatment and healing process. Usually surgery is a last recourse, as it generally has the same long term results as physical therapy. In fact, 9 out of 10 people with herniated discs will find that their symptoms resolve on their own over the course of days to weeks. Many people with herniated discs may not even realize that they suffer from the condition. Still, in certain severe cases, surgery may be needed. Usually in the course of diagnosis, the doctor will run you through a number of tests and diagnostics to identify specifically what the injury is, and whether it warrants surgical intervention.
Diagnostics for lower back disc herniation
X-Ray
Most people are familiar with X-Rays, and have likely had one at some point in their lives. X-Rays are usually the first round of diagnostic testing for injury scenarios because they are cheap and readily available. X-Rays are great for diagnosing bone injuries. However, they are not as useful in diagnosing a soft tissue injury such as a disc herniations. However, depending on the context of the injury, a doctor may still order an X-Ray to rule out other types of injuries, such as spinal fractures or other bone related ailments. If the X-Ray turns up a fracture or hard tissue injury of some kind, then the physician may go down the route of treating that injury before continuing on to investigating a soft tissue injury.
CT Scan
A CT, or Computerized Tomography scan is actually a series of X-Rays that builds a more complete image of the area than just a regular X-Ray alone. Similar to an X-Ray, a CT scan will not be able to identify soft tissue damage on its own. It can be used to help in diagnosing traumatic injuries, especially with special dyes injected into the body. However, it may not be sufficient on its own to diagnose a disc herniation. One thing that it can help with however is determining the size of gaps between vertebrae. This information can contribute to the diagnosis of degenerative disc disease.
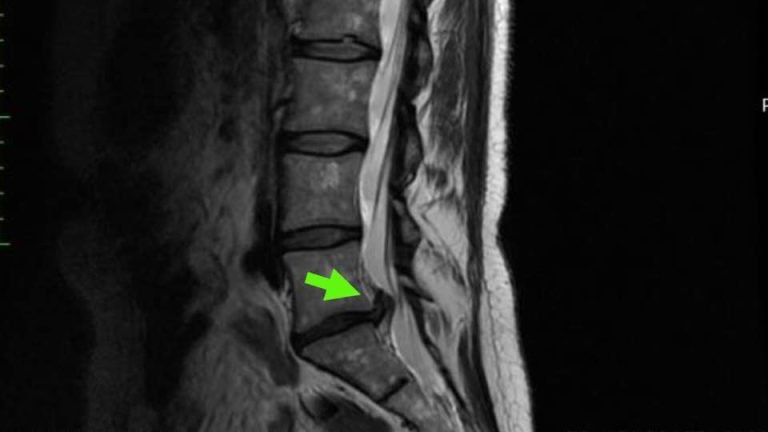
MRI
In many ways, an MRI is the gold standard when it comes to diagnosing a lower back disc herniation. MRIs do not rely on radiation for imaging. Rather, MRI’s generate images using magnetic fields, and are generally able to capture better images of internal soft tissue. The downside to this is that it can affect magnetic metals. While individuals with metal pins, screws or plates can usually safely undergo MRIs, those with more sensitive equipment such as pacemakers may not be able to have this type of imaging done. Like a CT scan, an MRI captures multiple images to create a comprehensive view inside of the body. Using this view, the radiologist can clearly identify soft tissue within the body, and whether any of that tissue is out of place, as in the case of disc herniations.
When Does Surgery Make Sense?
When pain interferes with daily activities
Chronic pain is both a physically and mentally challenging condition to deal with. It can interfere with your daily life, whether at a personal or professional level. For those who depend on their bodies to make a living, it can have financial repercussions, and even for those who are in white collar professions, it can be a constant distraction from workplace performance. The constant presence of lower back pain can also bring you down, and contribute to things like depression. This can influence your personal life as well. You may find yourself avoiding physically demanding activities with the people you care about. And even if you’re just casually hanging out, spikes of pain can ruin a fun time.
For all of these reasons, constant pain that interferes with your life is a valid reason that you might end up having surgery for lower back pain or disc herniations. A piece of soft tissue protruding into the nerves that run along your body can run the range from painless up to excruciating, and surgical involvement might be needed to relieve the worst cases. However, surgery and the recovery from surgery can both be painful affairs in their own right. Make sure you closely coordinate with your doctor to make sure that the risks of operating on your condition and the success rate from the procedure are justified by the impact of your lower back disc herniation.
Weakness or numbness
Pain in and of itself can be a bad enough condition, but weakness and/or numbness in association with a lower back disc herniation can be even more worrying. In this situation, the bulging disc is pressing on the nerves around the lumbar spine and lower back to the point where their function is being impeded. That is, due to the pressure from the soft tissue of the spinal disc, the nerve is unable to send signals from the brain to the body part, or vice versa, the body part is unable to return signals carrying sensation from the limb back to the brain. This can be a very serious situation, because if it persists for too long, the muscles that are controlled by the nerve can atrophy. That means that they shrink and become less functional, or even non-effective. Once this occurs, it is difficult to reverse. If you are experiencing pain or numbness after a lower back injury, make an appointment with a physician as soon as possible. The sooner that the cause of the weakness or numbness is identified and treated, the better the outcomes for the patient!
Difficulty with walking or standing
Difficulty with walking or standing may occur as a result of a lumbar disc herniation due to either pain or weakness. Walking and standing are important activities in day to day life, and if your only relief after injuring your lower back is to remain horizontal, then finding the motivation to go out and live your life can become a chore. If walking or standing are too painful, and this pain persists for a long time after your injury, then surgery may be the best way to resolve this issue. However, pain may not be the only reason that walking or standing become difficult. Similar to the weakness or numbness in the limbs of your lower body (or portions thereof), individuals with lower back disc herniations may experiencing difficulty with these activities if they can’t properly coordinate their movement. For example, some individuals with lumbar disc herniation experience what’s known as ‘drop foot’, where they are unable to properly raise their foot. They may find themselves tripping over themselves. People who rely on mobility to earn a living may need surgical intervention to maintain this mobility, and to make sure that they do not seriously injure themselves on the job.
Loss of bladder or bowel control
I think it goes without saying that loss of bladder or bowel control are serious issues that needs to be addressed immediately. Similar to limb weakness or numbness, the loss of these more messy bodily functions is due to impingement upon the nerve that controls them. This condition likely requires immediate medical attention, les your bladder or bowel control be permanently affected.
Individuals from all walks of life may experience lumbar disc herniations. Some are young, or in shape, and will notice immediate changes to their physical abilities. Such individuals may be much better at identifying when they need to seek medical assistance. However, other people, such as the old, infirm or obese may already experience a number of the above symptoms, and not think to seek medical aid. However, everyone should have the ability to live life to the fullest, and if that necessitates surgery, then the risks of undergoing invasive procedures as outlined in this article may be worth it. Sadly, not everyone is a good candidate for an operation. Anyone experiencing the above symptoms should certainly consider having their herniated disc fixed via surgical intervention, but not everyone experiencing these symptoms will be a good candidate. Surgery is a physically taxing procedure with many risks involved, and it should not be undertaken lightly. Generally only those who have attempted medication and/or physical therapy but not had success with those approaches should even consider it. Likewise, the best surgical outcomes for patients usually occur with healthy individuals. Those suffering from other health conditions may not get enough out of surgery to justify the risk.
Conclusion
Although surgery is daunting, most people with lumbar disc herniations will not need it. Most people can overcome their condition through rest, exercise and rehabilitation. For those that do need it though, it can help them avoid more serious complications that can arise through a lower back disc herniation, and return to their normal day to day lives. All of these treatment options should be undertaken under the supervisory care of your doctor.